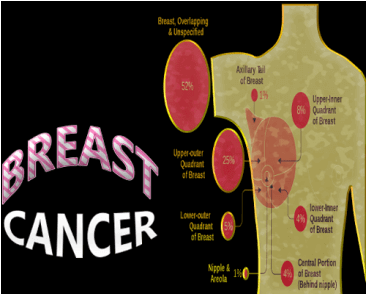
The most frequently encountered cancer in women is breast cancer.
BREAST CANCER
Description
The most frequently encountered cancer in women is breast cancer, an aggressive cancer which is responsible for 18 % of deaths due to cancers.The frequency increases with increasing age, so older women are more prone. Contrary to popular belief, men can also get breast cancer.
CAUSES
As with most cancers, the exact cause of breat cancer is not yet known. There are certain risk factors linked with the development of breast cancer in an individual. However breast cancer can also develop in someone with none of the risk factors present. Following are the risk factors:
- History of benign lumps in the breast
2. History of ovarian cancer
3. History of breast cancer in a first degree relative eg sister or daughter of a woman
4. Carrying genes BRCA1 and BRCA 2. The incidence is: about one woman out of 200 has these genes.
5. Women of African descent
6. Women above 50
7. Exposure to high doses of radiation
8. Too much estrogen in circulation
9. Early onset of menstruation, under age 12
10. Delaying childbirth so first born when woman is over 3011.Early menopause, by age 55
12. Menstruating less than or more than the average cycle
13. Diet includes too much fatty food
14.Obese women
15. Alcoholism
16. Mutations in genes eg BRCA1, BRCA2
17. Not having children
18. Women whose breasts are dense, with lots of connective tissue
19. Certain oral contraceptives
20. History of breast disease eg atypical hyperplasia
21. Positive family history
22. Smoking
23. Inactive lifestyle
SYMPTOMS
Breast cancer does not have symptoms in the initial stages. There is usually only a lump in the breast. However, only a specialist can find out if the lump is cancer or a benign mass. Other symptoms may include:Pain in the breast or axilla (armpit). This must be distinguished from normal tenderness a woman feels in her breast or axilla during or near her menstrual cycle.
2. Skin around the breast seems pitted, like an orange peel. It is called peau d’orange.
3. Redness of skin (breast area)
4. Rash seen on nipple (one or both) or around them
5. Lump in one or both armpits
6. Thickening of breast tissue to form a palpable mass
7. Changes in shape of the breast or in its size
8. Discharge from nipple with or without blood.
9. Scaly or flaky skin of breast or nipple
10. Nipple is inverted or seems sunken
DIAGNOSIS
In addition to taking a medical history and physically examining the breasts, the doctor may order the following tests:
- Biopsy
2. Mammogram
3. Bone scan
4. MRI
5. CT Scan
6. PET Scan
7. Blood tests
8. Chest X-ray
STAGING OF CANCER:
After diagnosis of cancer is made, the doctor will stage the cancer. Staging means determining the extent of spread of the cancer. Staging is done from Stage 0 to Stage 4 depending on the extent the cancer has spread or invaded the surrounding areas.
Stage 4 is the most advanced stage where cancer has spread extensively.
Another staging system is the TNM system. T stands for size of the tumor, N stands for nodal involvement ie nearby lymph node invasion and M stands for distant metastasis ie spread to other regions of the body. Treatment plan depends on staging of the cancer.
TREATMENT
Cancer treatment involves a team of doctors that work together with the patient. They include specialists like medical oncologist, radiologist, surgeon, nurses, counselor, nutritionist, social workers and pharmacist. Treatment also depends on the age of the patient and the growth of the tumor ie whether it is slow growing or aggressive and fast growing.
Other factors that influence treatment planning are the staging of the tumor and its subtype and genome markers. Patient’s menstrual history and whether or not she is menopausal need to be taken into consideration plus any know gene mutations in the breast cancer genes. Overall health of the patient will also determine prognosis.
For early stage cancer the best approach is surgical excision of tumor along with a wide margin to include healthy tissue. In some instances further surgery is required because microscopic cancer may be left in the breast or surrounding areas.
Cancers that grow quickly or are more widespread usually require neoadjuvant therapy which means treatment with hormones or chemotherapy followed by surgery.If the cancer has spread within the breast, a lumpectomy or a segmental mastectomy or a total mastectomy may be required.
Surgery may also be done on axillary lymph nodes or underarm area if needed to rule out cancer in these areas (nodal involvement). Sentinel lymph node biopsy is usually performed to check for cancer cells. If this biopsy is positive, then axillary lymph node dissection is done.
The next step following a successful surgery is adjuvant therapy which is done to minimize risk of cancer recurring if there are any malignant cells left behind.Such treatment consists of chemotherapy, hormonal therapy, radiation therapy and targeted therapy. Any one of these or a combination may be included in the treatment plan.
TARGETED THERAPY:
Targeted therapy means that the spread or growth of cancerous cells is inhibited, with fewer side effects than chemotherapy. The environment of the cells that nourishes the growth of cancer is targeted. Sometimes certain proteins that are responsible for the cancer or certain genes are targeted.
Sometimes the cancer is inoperable ie it cannot be removed via surgery. Then these other options are utilized.
RADIATION THERAPY:
As the name implies, certain types of radiation is used to eliminate cancer cells eg high energy X-rays. Radiation is emitted via a machine onto a patient’s body. This is called therapy using external beam radiation.
If radiation is delivered in the operation theater via a probe, the procedure is called intra-operative radiation. A radioactive substance may also be used to kill the cancer cells by placing it inside the tumor. This process is known as brachytherapy.
Radiation therapy is given in fixed doses for a limited time, following surgery and/or chemotherapy to minimize risk of recurrence. In some cases radiation is needed before surgery to shrink the tumor. This is referred to as neoadjuvant radiation therapy.
Common side effects of radiation therapy are:
1. hyperpigmentation
2. Swelling of tissue of breast
3. Redness of skin
4. Discoloration of the area
5. Skin peels off in the affected area
6. Blister formation
7. Fatigue
8. A rare complication is radiation pneumonitis.
CHEMOTHERAPY:
Chemotherapy means giving the patient drugs which eliminate the cancerous cells. They inhibit the cancer cells’ division and growth. These drugs are either given orally or intravenously (IV).
Sometimes chemo is given prior to a surgery which helps shrink a tumor and easier to operate upon. This is called preoperative chemotherapy. Adjuvant chemotherapy is given following a surgery to kill any remaining cancer cellls or if there is recurrence of the cancer.
Side effects of chemotherapy include:
1.Nausea and /or vomiting
2. Infection
3. Loss of appetite
4. Fatigue
5. Loss of hair
6. Diarrhea
7. Rare effects are nerve damage or damage to heart.
These effects are dependent upon the drug used in the chemo and the frequency of receiving it. These can be managed with supporting medicines.
The side effects stop when chemo is withdrawn.
HORMONAL THERAPY:
This therapy is referred to as endocrine therapy is used for those cancers that are ER-positive or PR-positive ie they have receptors for hormones estrogen or progesterone. These cancers use such hormones for their growth so this therapy is targeted at blocking of these hormones.
BREAST RECONSTRUCTION:
After a mastectomy a doctor, usually a plastic surgeon performs reconstructive surgery on the breasts to recreate the breast. Synthetic implants may be used for this purpose or tissue from the patient’s own body is used called tissue flap procedure.Implants can be filled with silicone or gel and replace natural breast tissue.However, there are side effects eg infection or pain in the area where the implant is.
The surgeon may opt for a tissue flap procedure eg Transverse rectus abdominis muscle flap, Deep inferior epigastric artery perforator (DIEP) flap, Gluteal free flap.If the patient is unwilling to go for reconstructive surgery, she can opt for an external breast prosthesis. Usually made of silicon, the artificial breast fits into a especially desgined mastectomy bra.
If a patient is at an extremely high risk of getting cancer, both breast may need a mastectomy. This is called bilateral mastectomy but there are a number of complications with this procedure so potential risks must be weighed against the benefits.
PROGNOSIS:
Long term outcome of the treatment depends on the cancer and how much it has invaded the surrounding structures as well as patient’s response to treatment. Terminal cancer is when the cancer cannot be treated or if it has spread to a point where it can’t be cured.
Counseling of the patient and the family is often needed to prepare them for the outcome and only palliative care can be provided at this stage to make the patient comfortable. Palliative care aims at easing the pain and other symptoms and offering physical and emotional support to the patient.